
The COVID-19 pandemic has had profound impacts on the weight loss and bariatric surgery industry.
Necessary shutdowns in elective surgery provision across the globe have led to blow outs in waiting lists for provision of bariatric services as these procedures are universally deemed “non-urgent”.
Effects of the pandemic on weight and lifestyle
The pandemic has had a negative effect on weight, mental health and lifestyle for those awaiting weight loss surgery(1). A survey from the United Kingdom involving patients with delayed bariatric surgery showed a marked increase in poor eating habits and reduced physical activity during lockdown. Mental health was almost universally worse with particular increases in anxiety levels. More than two thirds of patients in this group gained weight during lockdown.
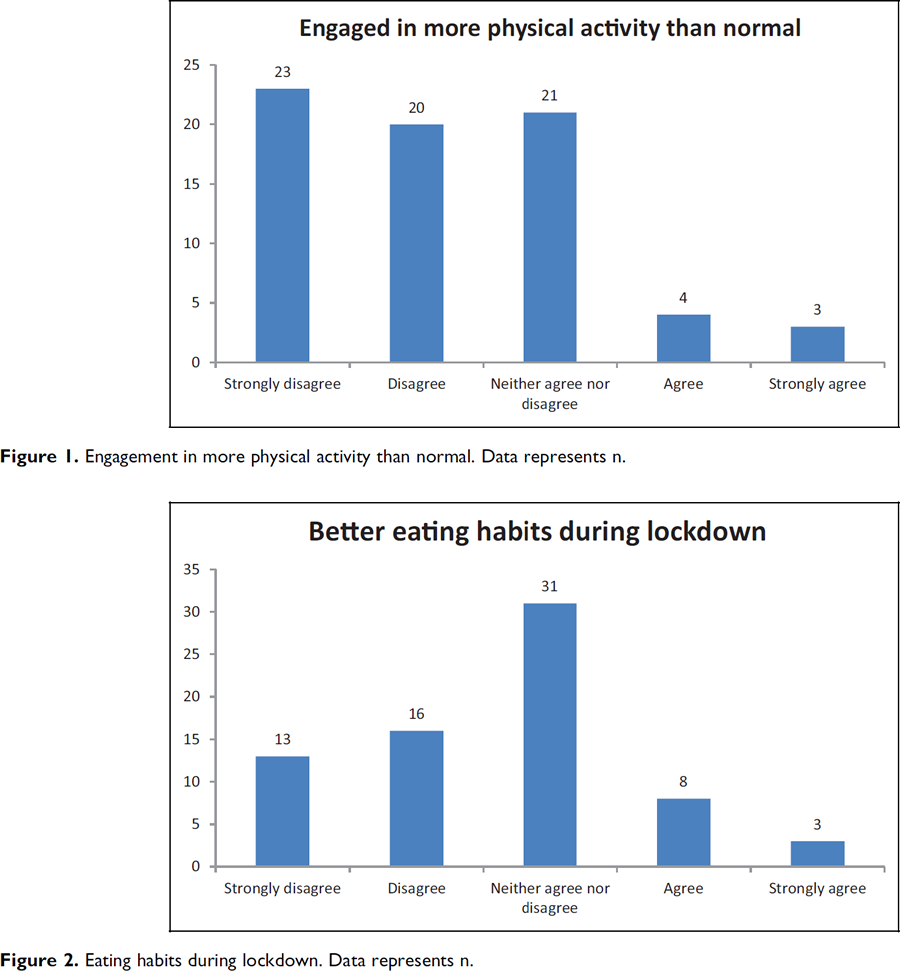
Impact of Obesity on COVID-19 infections
Unfortunately for those suffering obesity, outcomes from COVID-19 infection may be worse than those at normal BMI. (2) COVID will also impact more for those with advanced age and other metabolic diseases such as diabetes, high blood pressure, obstructive sleep apnoea and underlying heart disease. All of these medical conditions are themselves associated with obesity. The accompanying clearly demonstrates the increased risk of death from COVID as BMI rises.
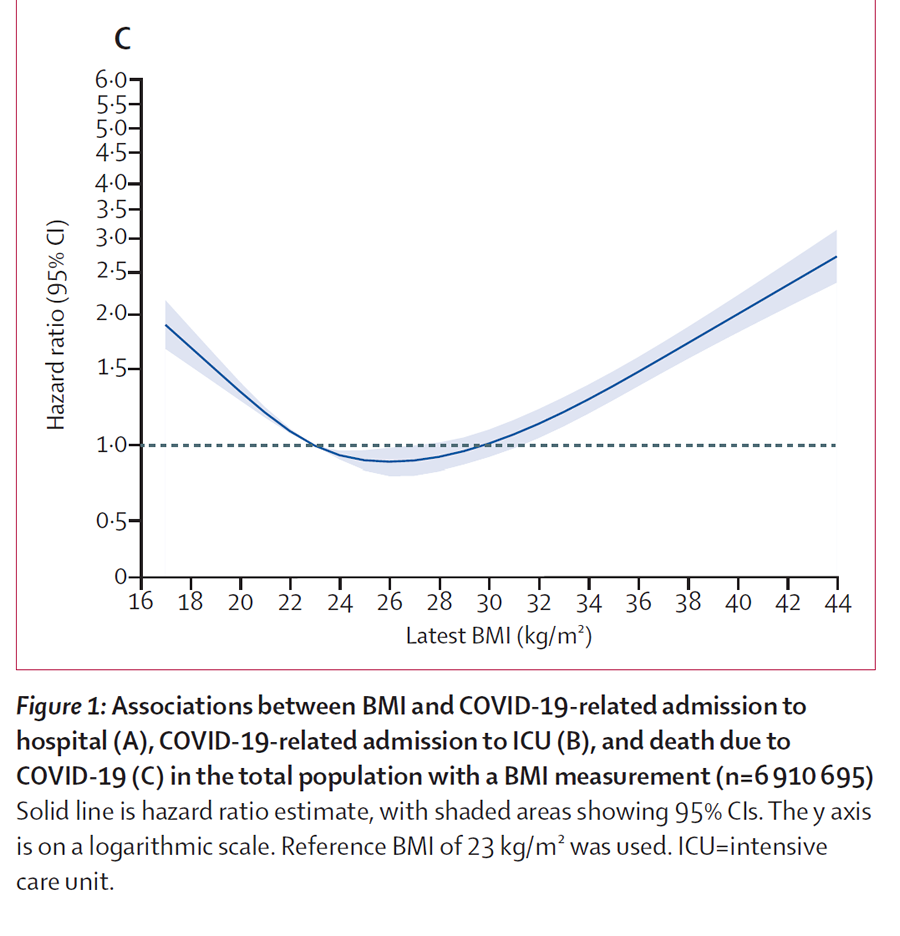
Bariatric Surgery and COVID 19
The reductions in bariatric procedures in the pandemic are related to maintaining staff, resources and equipment to treat COVID patients as well as freeing up ICU and other ward beds. Additionally is the reluctance to risk COVID infection during the recovery stage of surgery as well as reducing the risk of health staff contracting the disease from their patients.
The suspension of bariatric elective surgery has caused enormous anxiety amongst those who have planned their surgery for some time. Some are waiting for surgery in order to progress to the next stage such as hip replacement after weight loss or in some cases organ transplant.
Safety of surgery
Studies have been done looking at outcomes of bariatric surgery performed during the pandemic. An international study looked at 2116 patients undergoing bariatric surgery during the pandemic and found adverse effects and complication rates in a similar pattern to prior to the pandemic.(3) 10 patients were symptomatic with COVID during the 30 days post surgery however none had serious disease outcomes. Protocols in managing COVID risk (e.g. pre-operative testing) were thought to have a significant role in producing good outcomes.
Conclusion
Individuals suffering from obesity have had a challenging time during pandemic related lockdown. Well being, health and lifestyle have generally suffered for the majority and the postponement of planned surgery has exacerbated feelings of anxiety and reduced hope. We hopeful that pathways emerge whereby bariatric surgery and other elective procedures can be performed in a controlled and safe environment whilst we learn to live with the presence of the COVID-19 virus.
References
1. Ahmed B, Altarawni M, Ellison J, Alkhaffaf BH. Serious Impacts of Postponing Bariatric Surgery as a Result of the COVID-19 Pandemic: The Patient Perspective. J Patient Exp. 2021;8:23743735211008282.
2. Gao M, Piernas C, Astbury NM, Hippisley-Cox J, O'Rahilly S, Aveyard P, et al. Associations between body-mass index and COVID-19 severity in 6·9 million people in England: a prospective, community-based, cohort study. The Lancet Diabetes & Endocrinology. 2021;9(6):350-9.
3. Singhal R, Tahrani AA, Ludwig C, Mahawar K, collaborators G. Global 30-day outcomes after bariatric surgery during the COVID-19 pandemic (GENEVA): an international cohort study. Lancet Diabetes Endocrinol. 2021;9(1):7-9.